Patient Instructions - CPAP/BiPAP
Getting started with your CPAP/BiPAP
Table of Contents
What is Sleep Apnea?
Sleep apnea is a medical disorder in which a person stops breathing for short periods of time, while asleep. The most common cause of sleep apnea is an obstruction or blockage of the upper airway by weak throat and tongue muscles. This obstruction prevents the person from breathing fresh oxygen into their lungs and blowing out the carbon dioxide. An increase in carbon dioxide alerts the brain to resume breathing, causing a sudden gasp or snort. The struggle to move air in and out of the lungs past the obstruction and the rise in carbon dioxide disrupt sleeping patterns and make restful sleep impossible.
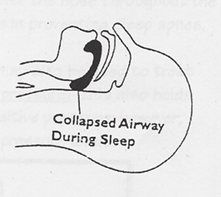
When a person with obstructive sleep apnea sleeps,
the tissues at the back of the throat collapse and block airflow of the lungs.
Symptoms of Sleep Apnea
- Restless sleep
- Chronic loud snoring with periods of silence
- Excessive daytime sleepiness with morning headaches
- Irritability
- Memory loss
- Fatigue and sexual dysfunction
- Depression
- Shortness of breath and choking through the night
- Increased risk of work related and automobile accidents due to fatigue
Sleep apnea symptoms may not seem serious, but this condition can affect daytime alertness and functioning which can cause a decrease in the quality of your life. If this disorder continues untreated more critical problems may arise, including: increased risk of stroke, high blood pressure, and heart problems.
Treatment for Sleep Apnea
- New oral laser treatments for airway obstruction
- Surgical reconstruction of the upper airway
- Noninvasive PAP therapy
Making PAP Work For You
What is PAP Therapy?
CPAP stands for "Continuous Positive Airway Pressure". It is the administration of a set amount of air pressure to hold open the airways, while you sleep. The air flow is delivered by a nasal mask worn over the nose throughout the night. The CPAP therapy is painless and very effective in preventing sleep apnea.
A similar modification of CPAP, called BiPAP, may also be used to treat sleep apnea. BiPAP stands for “Bi-Level Positive Airway Pressure”. This also holds open the airways at night by a continued supply of positive pressure; however, instead of one pressure, BiPAP creates two different pressure levels.
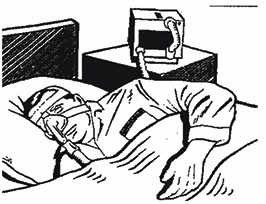
Equipment
- CPAP Machine
- Fitted mask with velcro headgear for a secure fit
- Tubing to connect the mask to the machine
- Humidifier (optional)
Use of Headgear and Types of Masks
- Nasal Mask - Triangular plastic mask that covers the entire nose and seals against the skin. It is bordered with pliable material for patient comfort. This is the most commonly used mask.
- Nasal Pillows - Small tubes held against the opening of each nostril, creating a seal. These are mostly used in patients whom cannot tolerate the mask.
-
Full Facial Mask - Plastic mask covering both the nose and mouth. This mask is usually used with patients that mouth breathe for better effectiveness.
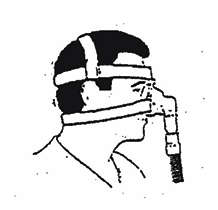
- Headgear - The headgear consists of a set of cloth and Velcro straps, which encircle the head to hold the facial mask firmly in place throughout the night. Correct adjustments of the headgear is the key to efficient air pressure delivery and patient comfort. A comfortable fit and a good seal may be established by adjusting the Velcro straps of the headgear. Once you have your headgear appropriately fitted, you should be able to slip it on and off fairly easily.
Setting Up Your PAP
Set up your PAP and mask will depend on the manufacturer of your machine. Observe all of the instructions for your particular unit.
- For safety precautions, place your PAP machine where it will not create a hazard, yet close enough to your bed so there will be plenty of slack in the tubing.
- All patients are advised to have a ground fault interrupter installed to protect the circuits in the bedroom and to install a surge protector. In normal use, the PAP will use about as much electricity as a light bulb.
- Add only distilled water in your humidifier chamber.
Cleaning Your PAP
Cleaning and Disinfecting
Patients are encouraged to clean the equipment in the morning, allowing adequate time for drying before the next use. Disassemble the PAP circuit. Wash all of the surfaces in a warm detergent solution. Rinse thoroughly. Leave equipment to air dry or you may assemble the unit and run air through the tubing, lessening the drying time. For an optional disinfecting technique, you may soak the equipment in one part vinegar to three parts water for one hour.
- Masks - Need to be cleaned daily and replaced if they become stiff, cracked, or broken.
- Tubing - Should be cleaned daily and checked monthly for leaks
- Filters - Wash reusable filters weekly and replace disposables monthly.
- Humidifiers - Should be cleaned daily with your mask and tubing.
Avoid Alcohol or Bleach Based Cleaning Products
Using either of the above may damage or destroy the plastics that make up the components of your PAP circuit mentioned above.
Preventative Maintenance
Your PAP unit may require a periodic assessment to maintain mechanical performance. Please contact MedCare for additional information.
PAP Treatment Benefits
- Less daytime drowsiness and fatigue
- Improved memory and concentration
- Better work performance
- Improved mood
- Less health risks, including high blood pressure and stroke
- Less risk of motor vehicle and work related accidents
Common Questions and Concerns about PAP
My nose and throat have been dry and sore since I started using my PAP, what can I do?
The excess air flow from a PAP tends to dry the tissues lining the upper breathing passages, including the nose and throat. This can lead to irritated, crusty and possibly bleeding airways. A simple solution is the use of a humidifier or saline nose drops to keep the airways moist.
The mask for my PAP has been causing a rash around my nose and swelling under my eyes, what can I do?
Skin irritation from a mask that is too tight can be common. The excess pressure exerted on the face may cause skin deterioration or break outs. The best way to prevent this is by keeping your skin clean and a daily washing of the mask. If the mask seems too tight, the headgear may need to be adjusted, or a bigger mask used. Also, “baggy eyes” may indicate too large of a mask. Air blowing into your eyes throughout the night may cause eye drying and irritation. Some small leaks are inevitable, but are usually compensated for by the PAP unit. Physical discomfort from the mask and headgear can limit the effectiveness of the PAP.
Should I take my PAP on vacation or on business trips with me?
Almost immediately after stopping use of their PAP, most patients resume sleep apnea and snoring. The best choice, if traveling, is to take your PAP with you. The majority of PAP units are small enough to carry onto an airplane and can be stored under your seat. Remember to take all of your equipment and electrical adapters as needed.
PAP/RAD Compliance Information
Your insurance company requires MedCare to obtain a compliance reading of your Pap/Rad unit for average hours of use. Most insurance companies require this information for final payment and/or continual rental of your unit. MedCare is using wireless modem technology to obtain this information. This modem will regularly call in hours of use for our records. Between sixty and ninety days we should have enough compliance information to present to your insurance company. Adherence to therapy is defined as use of PAP/RAD ≥ 4 hours per night on 70% of nights during a consecutive thirty day period. This report will then be forwarded to your insurance company for review and ultimately final payment and/or continual rental of your unit.
At the end of your 90-day trial period if you have not met the therapy requirements as set forth by your insurance company, payment on your behalf may or will be denied and you are responsible for the costs associated with the device.
A face-to-face re-evaluation by the treating physician may be needed for coverage beyond the three month rental period. You must check with your treating physician to schedule a return visit no sooner than the 31st day but no later than the 91st day after your PAP set-up. Failure to do so may result in denial of coverage.
MedCare Follow-Up and Resupply Program
Once it has been determined that you are compliant with your PAP/RAD device you will be eligible for replacement supplies through your insurance company. You will receive a live call from a MedCare representative when you’re eligible for replacement supplies every three months. If you need supplies before the call cycle, you may contact MedCare for the items needed.
The insurance company typically replaces supplies as follows:
| Product | Eligibility | Product | Eligibility |
| Mask | 1 Every 3 Months | Chinstrap | 1 Every 6 Months |
| Tubing | 1 Every 3 Months | Full Face Cushions | 1 Every Month |
| Water Chamber | 1 Every 6 Months | Nasal Cushions | 2 Every Month |
| Headgear | 1 Every 6 Months | Nasal Pillows | 2 Every Month |
| Disposable Filters | 2 Every Month | Pollen Filters | 1 Every 6 Months |
If you have any problems, questions, or concerns about your PAP device, please contact MedCare.